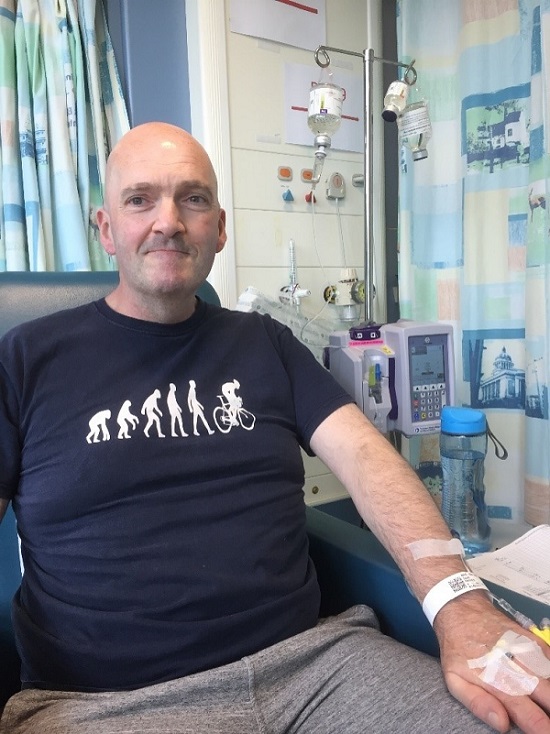
Scott was the 9th patient in the UK to participate in a CAR T-cell therapy trial, following a relapse from Acute lymphoblastic leukaemia (ALL). Scott shares with us how this treatment option became available, what led to this decision and how it was successful for his ‘dream outcome’ of remission. CAR T-cell therapy has been approved to treat children and young adults with B cell acute lymphoblastic leukaemia and adults with large cell lymphoma living anywhere in the UK. In both cases, it’s only offered after other treatments have been unsuccessful. For more information, check out our CAR T-cell therapy page.
Can you describe how you got diagnosed with ALL?
I went to my GP for the first time in 5 years as I’d been feeling unwell. I’d lost weight without trying and I was sweating excessively during the night. All I wanted to do when I got home from work was sleep and I had glands in my neck which had swelled up to a size to rival Mike Tyson in his prime! One day at work during a presentation, I passed out and fell to the floor.
I went to Queen’s Medical Centre in Nottingham and was kept in overnight for observation and tests. At Nottingham City Hospital haematology department the next day, the consultant explained that I likely had leukaemia, specifically Acute Lymphoblastic Leukaemia (ALL). A biopsy later confirmed what was suspected.
Only when you have been given the news that you have cancer can you begin to imagine how your life will never be the same again.
What treatments did you initially have?
My hospital stays got longer and the treatment more severe. My body responded quite well to chemotherapy and radiotherapy, so I was allowed home frequently. I had my stem cell transplant in August, thanks to stem cells donated by an anonymous UK male on the Anthony Nolan register. This meant I was in remission! A few weeks later, I was sent home to recover and be monitored.
How did you cope during this period?
I decided that should I make it out of the hospital bed, I would buy a bike to get back to life. All went well in remission for the next 18 months. Slow but steady progress saw me riding my beloved Carrera Virtuoso bike around my local area and much further afield.
What led you to decide to have CAR T-cell therapy?
A call from my transplant nurse in February 2018 changed the whole journey once again. A routine three month biopsy result showed positive again for leukaemia - it had returned for a second time as a relapse.
I had two options laid out very clearly to me. The first was to undertake conventional relapse treatment of a month of continuous chemotherapy, with the hope of remission for an unknown period of time. Or I could agree to sign up for a trial at UCLH in London.
The trial was looking at a treatment called CAR T-cell therapy. It had evolved in the US with some really encouraging results over the last few years in both lab trials and with real patients.
If I agreed to participate in the trial, I would be only the ninth person in the UK to do so.
When you are looking into the abyss and someone throws a rope to you, human nature and the will to survive will make you reach out and cling on to it with all strength. So my wife and I found ourselves on our way to UCLH a week later.
What did the CAR T-cell therapy entail?
The medical trial team at UCLH were the most positive and upbeat bunch of driven professionals. The consultant using the classic A4 pad showed me how the cell therapy would be done.
The T-cells taken from my donor would be engineered in the lab to have a coating, called ‘Chimeric Antigen Receptors’ or ‘CAR’ put on the surface. These cells would then be put into me with the intention of finding and killing the specific CD19 leukaemia cells in my system. Effectively, a war in my blood of good cells hunting out and taking out the bad ones.
The downside, as my consultant explained, was that the level of toxicity to me during the treatment was largely unknown, hence the need for trial patients. However as far as the team were concerned, the upside to all the unknowns was the possibility that this would mean remission, achieving the ‘dream outcome’.
How did the CAR T-cell therapy go?
The trick was now to keep me alive with an intense regime of chemotherapy until the cells were ready, which could be many months away.
The start date of 31 July 2018 will stay with me always. I had to go into isolation for 10 days before for prepping and body conditioning. Then, at 12 noon on the 31st, a team of seven arrived in my room, pushing a steel cylinder.
A simple bag of cells were placed in a small tub of water until they reached room temperature. The bag was then attached to a pump and infused into my arm. My CAR T-cell journey began.
What was the result?
A week later I was given the news that cells had been detected doing their thing in my blood. The euphoria was indescribable. Over the next few days I was closely monitored and then told simply I could go home!
I’ve been in remission ever since. I still visit UCLH every three months for a check and biopsy. I‘ve now joined a local cycling club (Ilkeston CC) and in June I completed my first organised Century 100-mile ride.
To sustain the miles over nearly nine hours of continuous pedalling is a testament to the hard work and dedication put in by hundreds of people who have shaped this journey. The medal I received after the ride now symbolises my new journey back to life.
Current status of my remission: still turning over those pedals…
If you or someone you know is going through a stem cell transplant and would like more support, we’re here for you. To find out more, visit anthonynolan.org/patients